Depleted of needed energy, our body’s cells can’t complete all their designated tasks. Organs no longer function optimally, and we become exhausted. Energy levels often decline in disorders associated with aging, but with proper bodily maintenance this doesn’t have to be the case. One of the main robbers of energy is mitochondrial dysfunction, which is seen in various conditions that develop in later life such as Alzheimer’s disease.
The Mighty Mitochondria
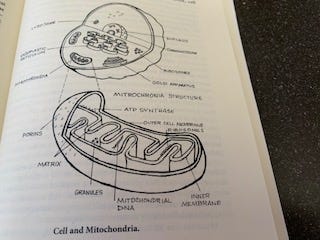
Mitochondria are microscopic structures within our cells that store energy. Mitochondria break down the food we eat and convert it into adenosine triphosphate (ATP). ATP is a vital source of fuel for not only cells but for our muscles, brain, and other organs. The co-vitamin CoQ10 is a natural substance used by mitochondria to produce ATP. COQ10 levels are decreased by statin cholesterol-lowering drugs and they decline with age. Low levels are also seen in many diseases, with the lowest levels occurring in hyperthyroidism.
Mending and Preventing Mitochondrial Dysfunction
Supplementing with 100 mg or more of CoQ10 increases mitochondrial energy and mental clarity, and it helps prevent mitochondrial dysfunction, a condition associated with Alzheimer’s disease and other neurological conditions. The antioxidant pyrroloquinolone (PQQ) works well with COQ10 because it stimulates the formation of new mitochondria and decreases lipid levels. Dietary supplements of 10-20 mg PQQ are recommended. An article in the Journal of Nutritional Biochemistry reports that PQQ also improves cell signaling pathways and reduces inflammation. Higher levels of PQQ are associated with lower levels of C-Reactive Protein (CRP), a marker of inflammation.
According to Garth Nicolson, a researcher in the Department of Molecular Pathology at the Institute for Molecular Medicine in California, CoQ10, PQQ and other supplements are needed to restore mitochondrial function. Other beneficial supplements include vitamins C, D, E, B1 and B2; the minerals magnesium, calcium and phosphate; the metabolites creating and pyruvate; the cofactors alpha lipoic acid, NADH, NAD and its precursor nicotinamide riboside, and nicotinic acid; the transporter L-carnitine (or acetyl-l-carnitine); the antioxidant glutathione or its precursor N-acetyl cysteine (NAC); and the herbs curcumin and schisandrin. I regularly take all the supplements mentioned. I began taking supplements in my 20’s after meeting an elderly lady at the Toledo Zoo who seemed full of energy. I thought She was in her 60’s although she had just turned 80. She said she took that old dietary supplement Geritol and credited it with her good health. I noticed a world of difference within days of starting a multivitamin.
Exercise and Exercise Recovery
It’s long been known that people who eat nutrient-rich diets and avoid refined sugars and processed foods, and who exercise regularly live longer, especially those who exercise regularly in middle age. Exercise allows us to retain mobility and balance, helping prevent falls and increasing stamina.
And it’s not just an increase in lifespan but in healthspan. Studies show that exercise causes cells to produce more of the proteins needed to produce mitochondria. Increases in mitochondria are seen in all forms of exercise but particularly in high-intensity interval training and in aerobic exercises such as walking and biking. Exercise also increases levels of AMP-activated protein kinase (AMPK). AMPK helps regulate cellular homeostasis, meaning it promotes optimal cell function. AMPK instructs cells to stop storing and burn stored fat for increased energy.
With age, exercise must be done safely to be beneficial. Recovery from exercise is also especially important to help maintain healthy muscles and joints. Recovery consists of proper stretching and cooling down and adding various dietary supplements. The anthocyanins are potent antioxidant phytochemicals found in dark colored fruits, particularly dark cherries. Dark cherry extract has long been used to reduce symptoms in gout, and it also helps speed muscle recovery after exercise, relieving post-workout stiffness. Cutch tree, Chinese skyllcap, white mulberry and the herb boswellia are also reported to relieve pain as well as ibuprofen. Theaflavins found in tea help and the antioxidant quercetin found in citrus fruits, helps rid the body of aging cells, which, in turn, helps combat the cellular effects of aging.
Diet
So far, on my program of intermittent fasting that I described week I’ve lost a few pounds and have been more motivated to exercise as I envision my telomere length increasing by leaps and bounds. I can only surmise that my former habitual daylong snacking was playing havoc with my insulin level and depleting my energy. Nutritional research supports my assumption. While I still manage to eat a bit of chocolate daily and drink red wine (for resveratol) at dinner I’ve lost my desire to snack in between meals.
Expert’s tips for increasing energy with diet include avoiding energy drinks, refined sugars, and artificial sweeteners and following a Mediterranean style diet based on whole foods, with ample fiber from fruits, vegetables and grains.


I'm in two Facebook groups for persons diagnosed with Graves'. One day in discussing intermittent fasting, we found that for a significant number of us our Graves' was "triggered" when we started an IF program. This was true for me as well. I emailed a researcher/physician who has studied IF (sorry I forget his name just now, but I could probably retrieve it buried in my email files) and asked him if he knew of any correlation. He answered "no," but also added that doing an epidemiological study would be pretty impossible. I seem to recall his saying as well that IF should actually improve metabolic profile. I had one hypothesis of my own about it. Dr. Eades of Protein Power claim to fame has written that body fat can store toxic components, as well as estrogen, and that losing weight can release these, with the estrogen triggering hormonal responses in women. ( don't know what the story would be for men.) I was doing quite well on IF, dropping pounds steadily, and tolerating the IF fairly well. I'd have to recheck my diary, but I think I was doing 5:2. I have wracked my brain for what my Graves' trigger might have been, as I have no familial background, so the IF remains one hypothesis. Also, my Graves' occurred very late as I was 71. The other hypotheses--possibly stress, but nothing truly dire, or possibly DES used by my mother in late 40's, but other than you mentioning this in one of your books, I haven't seen any definitive information on this. Anyway, I thought I'd mention this.
There is a connection with dieting and diet pills with Graves’ disease but dieting isn’t a cause. Most everyone with Graves’ disease has an initial hypothyroid. It’s usually mild and not diagnosed but some patients have overt hypothyroidism and are on thyroid replacement hormone for years before developing hyperthyroidism. Patients often don’t recognize the hypothyroidism until, in retrospect, they admit to having trouble with weight gain before developing hyperthyroidism. Diet pills containing amphetamine can be a trigger since they raise T4.
Graves’ disease is caused by a combination of genetic and environmental factors. The genetic factors overlap with rheumatoid arthritis, type 1 diabetes and lupus. Someone in your family have had one of these disorders. Or relatives may have had the genetic predilection but weren’t exposed to environmental triggers. These triggers include stress, antibiotics, infections, seasonal and food allergens, excess dietary iodine, and really anything that triggers an immune response.